Chronic Venous Insufficiency (CVI) Management

What is CVI?
Chronic Venous Insufficiency (CVI), also known as Ambulatory Venous Hypertension, is caused when valves in veins become faulty, leading to swelling in the legs. It can be managed with lymphatic massage and compression stockings.
How CVI Causes Swelling
In a healthy vein, blood passes through the valve moving upward toward the heart as the heart beats (pushes blood).
When the heart rests, the valve closes preventing blood from flowing backwards in the vein.
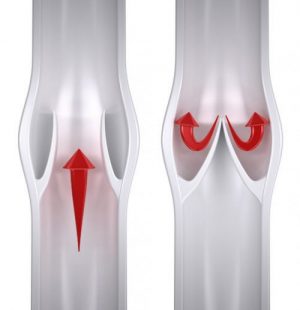
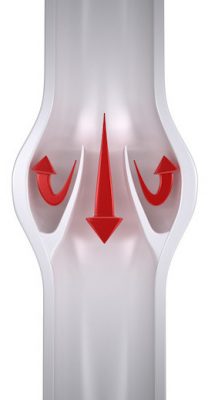
In Chronic Venous Insufficiency the valves are faulty meaning that blood does not advance towards the heart, but instead pools in the legs.
The reason that this condition is called Ambulatory Venous Hypertension is that as we are up and walking (ambulatory) there is more downward pressure exerted on the veins.
Because this pressure is greater than what would be found in a normal vein due to the larger amount of blood that isn’t being returned to the heart it is referred to as “hypertension,” or excessive pressure.
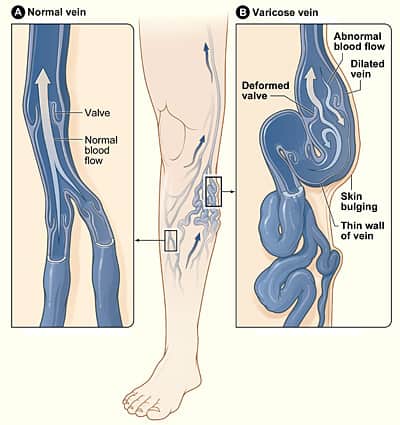
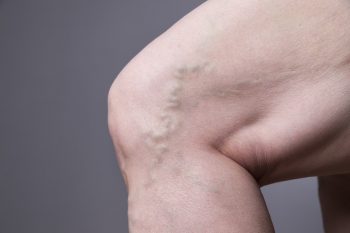
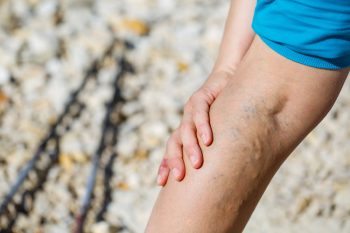
This excessive pressure over time distorts the shape of the veins leading to the formation of varicose veins.
These are the veins we can see through the skin that have a twisted and bulging appearance. Again, this bulging is due to them being under constant pressure from backflow that is happening due to valves above having failed..
Although a tendency to have varicose veins can be hereditary, people who are often on their feet, who regularly lift heavy objects, or who are or were pregnant are likely to develop varicose veins.
Let’s now take a look at what is going on at the microscopic level.
When blood rushes backwards in the veins (blue in the picture), more fluid diffuses (comes out of) the capillaries. The capillaries are the purple structures between arteries (red) and veins in the picture below.
Capillaries have “window-like structures” that allow things like nutrients to diffuse out of our bloodstream to feed the cells.
When there is excessive back pressure from blood that can’t make it up the veins in the legs, these capillaries become like a perforated garden hose and spray fluid out into the space between the cells.
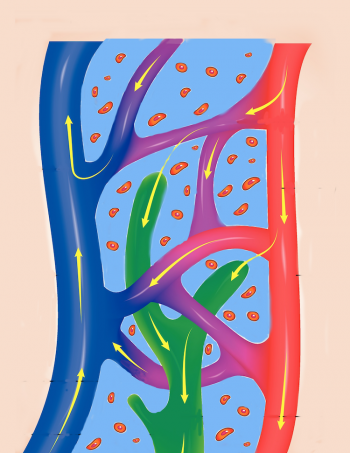
This excess fluid between the cells is normally removed by the lymphatic system.
The lymphatic system may be working fine, but there is simply too much fluid for the lymphatic system to keep up. We recognize this overabundance of fluid between the cells as a phenomenon we call swelling.
It is the job of the lymphatic system (pictured here in green) is to remove this fluid. However, Chronic Venous Insufficiency can produce more fluid than the lymphatic system can take up. This is similar to too much traffic trying to all take the freeway home at 5:00 PM. There are more cars than there is space on the road.
Stages of Chronic Venous Insufficiency
Stage 0: No swelling is present, but the veins are having some trouble returning blood to the heart. While there is more fluid leaking out of the capillaries into the tissue, the lymphatic system is working harder and removing the fluid fast enough that it does not accumulate.
Stage 1: Swelling (edema) is present and is visible, but it reduces or is completely eliminated overnight. In Stage 1, the veins are worsening, and while the lymphatic system is still 100% functional, the amount of excess fluid in the tissue is more than the lymphatic system can remove in a best-case scenario. The fluid in the limb is low in protein and does not cause changes to the surrounding tissues.
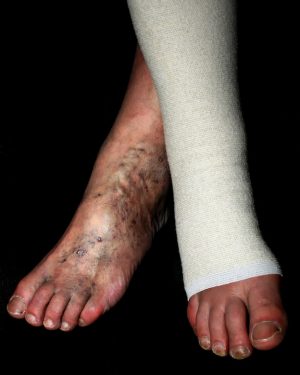
Stage 2: Swelling is no longer improving overnight. The lymphatic system has now become damaged by the constant need to work at 100% capacity. So, in addition to the continued worsening of the veins and the resultant increase of fluid leaked into the tissues, the lymphatic system is working at a reduced capacity causing a protein buildup in the tissue. This is a form of lymphedema called “phlebo-lymphedema.” This protein buildup leads to skin and tissue changes, usually in the form of hardening (fibrosis), color changes known as hyperpigmentation (usually red or brown) appear, and a state of chronic inflammation called stasis dermatitis can form.
Stage 3: This stage is characterized by all of the symptoms of Stage 2, plus ulcerations are present. These generally occur on the inside of the lower leg near the ankle.
Video Explaining Venous Related Lymphedema
(Phlebo-Lymphedema)
Management of CVI
Lymphatic Massage, or Manual Lymphatic Drainage (MLD) are used to treat swelling that results from Chronic Venous Insufficiency (CVI).
Left untreated, this swelling can result in a special form of Lymphedema called Venophlebic Lymphedema.
Lymphatic Massage (MLD) Removes Fluid Buildup
Although the cause of swelling related to CVI is not lymphatic in origin, Lymphatic Therapy reduces the swelling in the legs by painlessly removing the fluid caused by the backup of blood in the venous system.
Studies have shown that lymphatic drainage can significantly improve and often eliminate the symptoms (like venous ulcers) of CVI when performed regularly. It does this by improving lymphatic flow which reduces stagnation of fluid in the tissues. Together with walking while compressed, this is an excellent way to maintain Chronic Venous Insufficiency.
Compression Stockings
Compression stockings for long-term wear are a great adjunct therapy to improve symptoms of CVI.
You can be fitted for appropriate stockings at Pain & Swelling Solutions.
Many people object to wearing compression stockings because they think that they are all ugly, but there is a surprisingly wide array of styles and colors available. There are many samples for you to see and touch when you come in for your appointment.
Another problem that people who have tried compression stockings in the past tend to complain about is the fact that compression stockings are so hard to put on – and if you are trying to put them on like a regular stocking, that is certainly true.
However, there are lots of tricks to putting on compression stockings easily, including turning them inside out first and using special gloves to give you a better grip. These tricks along with a little practice make it so much easier that you really won’t mind putting on your stockings.
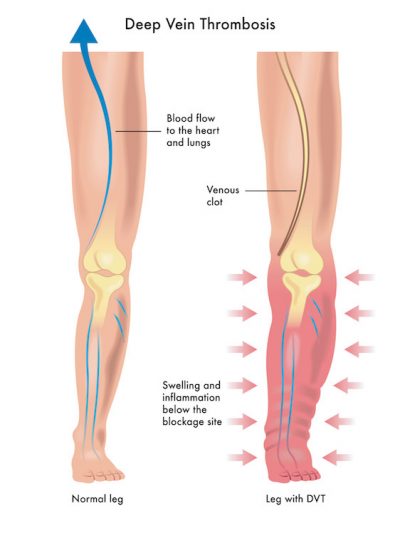
Some people who have Chronic Venous Insufficiency can develop what is known as Deep Vein Thrombosis, or DVT. This is especially true for people who tend to be more sedentary and for those people who do not wear compression socks regularly.
If you suspect you have a DVT you should seek immediate medical care. Signs of a DVT are: sudden swelling in the leg, pain or tenderness in the leg, warm skin on your leg, red or discolored skin on your leg, and veins that are swollen, tender, and/or hard to the touch.
If you have been told by your physician that your DVT is stable, your doctor likely prescribed compression stockings. Pain & Swelling Solutions can help you find the right stockings for you.
Note that Lymphatic Drainage is not advised for someone with a DVT – at least until they are on clot busting drugs and have physician clearance.